News
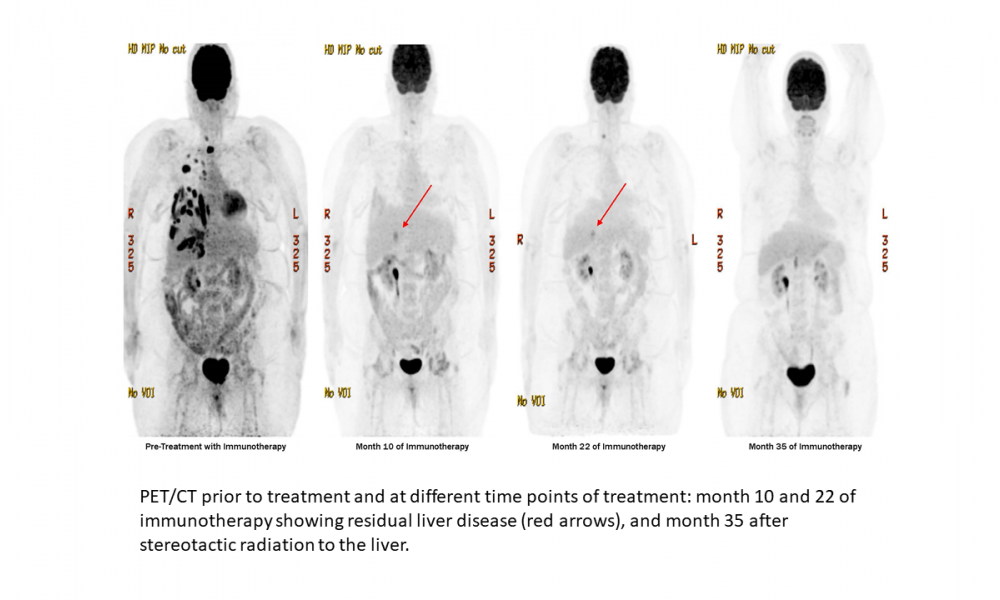
Genomic Analysis of Uveal Melanoma Case with Good Response to Therapy
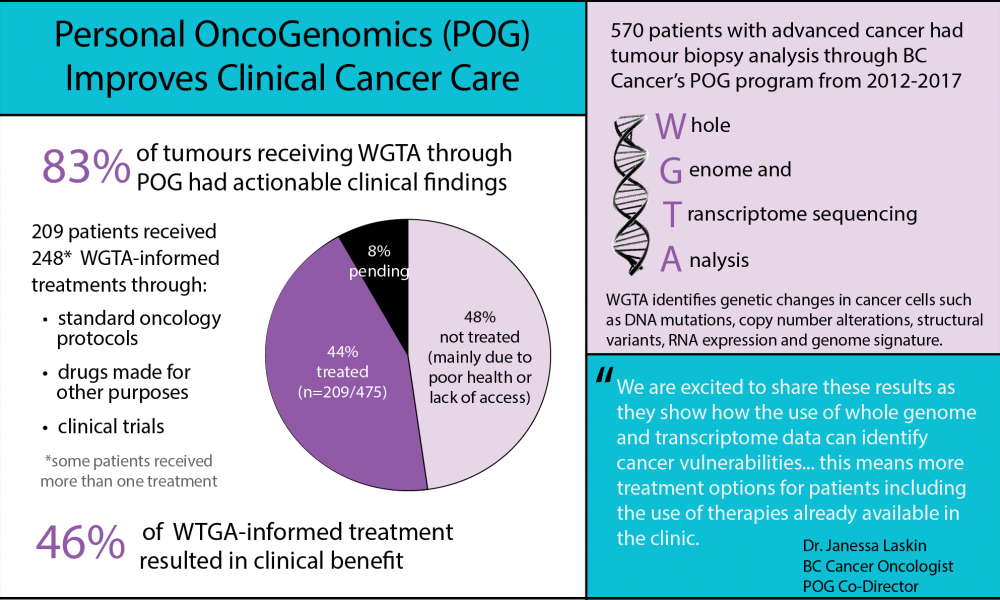
Whole Genome and Transcriptome Analysis Benefits Clinical Cancer Care
Genomic Analysis of Adrenocortical Cancer Identifies Treatment Targets

Evaluating whole genome transcriptome analysis for cancer biomarker discovery and diagnosis

New animation makes cancer genomics understandable for everyone
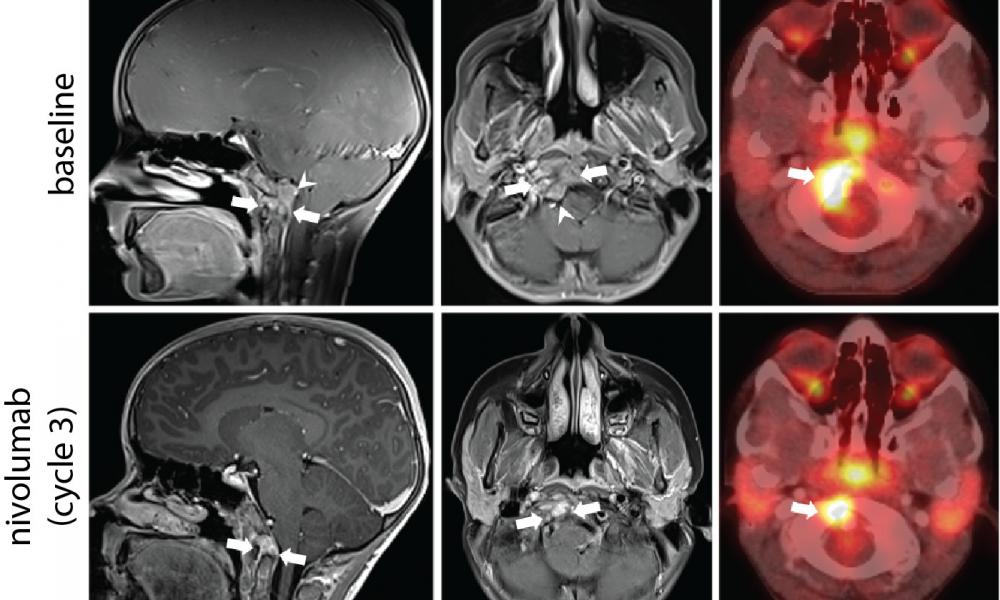
Treatment of pediatric chordoma with an immune checkpoint inhibitor slows tumour growth
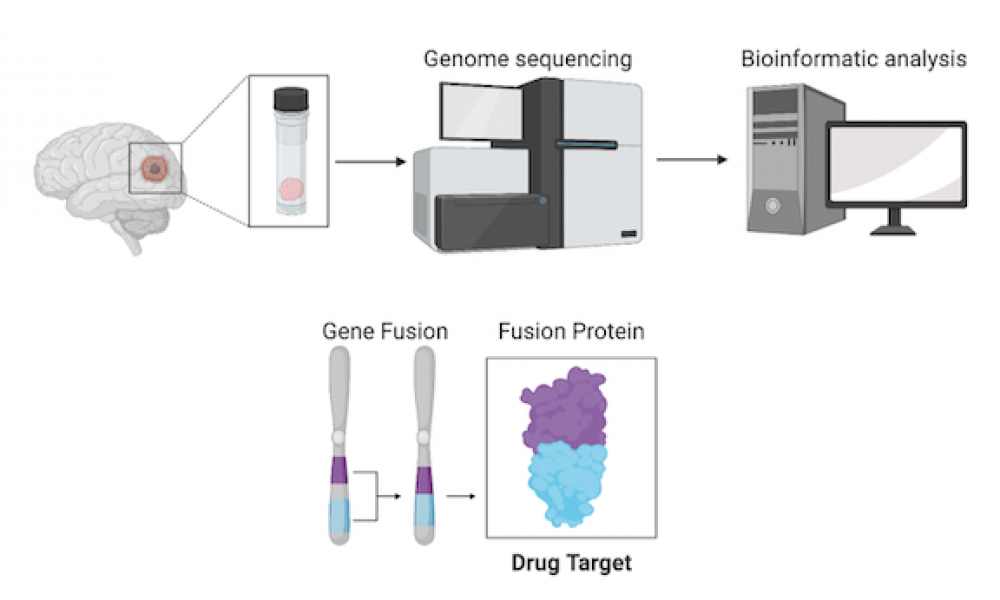
Pediatric case study demonstrates value in whole genome sequencing for cancer treatment planning
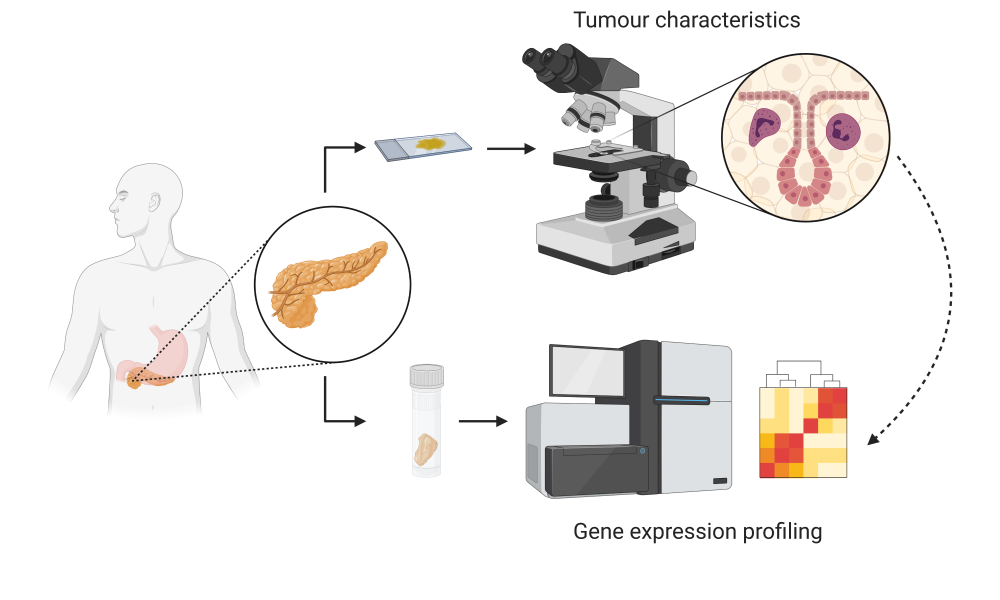
Molecular subtypes of common pancreatic cancers can be predicted from tumour characteristics
Gene expression analysis of pancreatic ductal adenocarcinoma (PDAC) tumours enables clinicians to stratify patients into molecular subgroups and select treatments that are best suited to each type; however, molecular subtyping remains cost-prohibitive and is not yet part of routine cancer care.
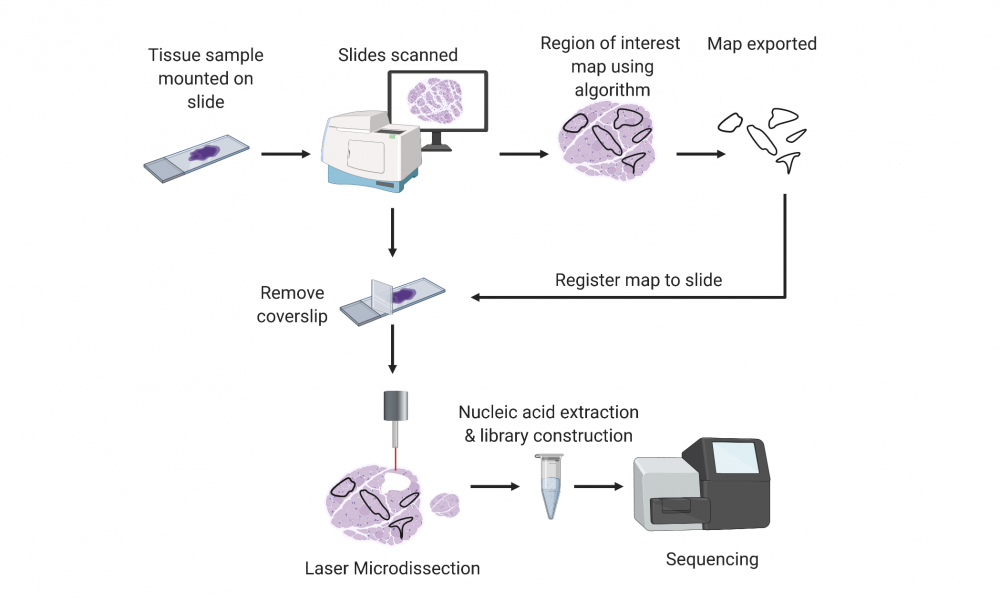
A machine learning algorithm for automated tumour sample processing
As researchers work towards establishing whole genome and transcriptome analysis into clinical practice for cancer care, scientists at the GSC continue developing innovative laboratory methods to improve efficiency and accuracy.
Canada’s Michael Smith Genome Sciences Centre respectfully acknowledges that we operate on the traditional, ancestral and unceded territories of the xʷməθkwəy̓əm (Musqueam), Səl̓ílwətaʔ/Selilwitulh (Tsleil-Waututh), and Skwxwú7mesh (Squamish) nations who have cared and nurtured this land for all time. We give thanks, as uninvited guests, to be able to live and work on these lands.